The causative agent of genital herpes is the ‘Herpes Simplex Virus’. Genital herpes is a usually sexually transmitted viral infection that involves the genital area in women and men.
Genital herpes is a usually sexually transmitted viral infection that involves the genital area in women and men. It is characterized by the appearance of ‘herpes’ lesions in and around the genital area, which are identical to those appear around the lips or mouth area. For this reason, the disease is also known as ‘genital herpes infection’. When the patient is infected with the disease, it manifests itself with blister-like lesions on the red surface, and causes complaints such as pain and itching in the genital area, groin pain, and burning sensation during urination.
Genital herpes infections are seen around the penis in men, around the vulva (external genital area),vagina in women, and also rarely around the hip and anus in the both genders.
The causative agent of genital herpes is the ‘Herpes Simplex Virus’. It is abbreviated as HSV. Once the body is infected with the virus, it may not cause complaints immediately. The virus first settles into the cell and manifests itself with attacks from time to time depending on the resistance of the immune system.
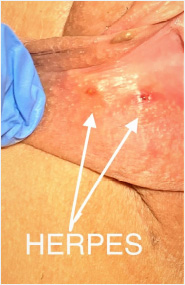
HSV is the most common cause of sexually transmitted genital ulcers. As a DNA virus, it has two different types as HSV-1 and HSV-2. The both are similar to each other in terms of their structures, but some tests can be distinguishes each of them.
Type 1 Herpes (HSV-1)
It is the most common type of HSV, which usually causes an infection in the lips, mouth, and face. It is commonly encountered in childhood. It is transmitted as a result of contact with infected saliva. Type 1 HSV infections, which usually occur in around the mouth, can rarely involve the genital area. Especially in recent years, an increase has been observed in such involvements.
Type 2 Herpes (HSV-2)
As a sexually transmitted virus, it is the main cause of genital herpes. Its prevalence increases in adulthood, when people begin to be sexually active. Factors such as the presence of a large number of sexual partners, other sexually transmitted infections, and having the first sexual intercourse at an early age increase the risk of genital herpes.
Ones the virus enters the body, it first settles in nerve cells. It remains latent there throughout life. It manifests itself with episodes of attacks.
Herpes attacks occur more often, especially during periods when the immune system is weakened. These include;
Herpes attacks are more commonly observed in people with chronic diseases, those who use chronic medications, those with low body resistance, those with malnutrition, those with insomnia problems, and those with bad habits such as smoking and alcohol consumption.
No. Genital warts are a different sexually transmitted infection caused by HPV infection. Genital herpes is caused by HSV infection.
Genital herpes has similar symptoms in men and women. It differs depending on whether it is a ‘primary’ (for the first time) or ‘recurrent’ infection. It may manifest itself with severe pain, or may show no symptoms.
It is the first encounter with HSV. Due to the body’s deprivation of antibodies against this virus, the complaints are severe. The incubation period (the time that elapses between the body’s exposure to the virus and the moment when the first symptoms appear) is 3-7 days on average. In other words, the virus does not show symptoms immediately after entering the body. During this period, it does not infect other people. The first symptoms appear within 2 weeks on average. These are, respectively, redness, itching and tingling sensation on the skin, then the formation of painful vesicles (blisters),then the burst of the vesicles and their turning into painful ulcers (wounds). At the last stage, these ulcers dry out, form scabs, and heal usually leaving no scars.
It is the transmission of HSV-1 to a person with antibodies against HSV-2, or the transmission of HSV-2 to a person with antibodies against HSV-1. Symptoms are milder than that of primary infection. This is because the pre-formed antibodies provide protection (even if partially) against the other type.
It is a condition where the patient has previously encountered HSV and already has antibodies. It has short-term, milder symptoms, which last 3 days on average. Itching can be the only complaint. However, if there is no improvement in a period longer than 7-10 days or if the lesions get worse, the patient should consult a physician.
Ulcers that occur in genital herpes infections usually do not leave a scar. Full recovery time is 2-6 weeks on average. During this period, the genital area is edematous due to vesicles. It also makes it difficult to urinate due to pain.
If the patient encounters the disease for the first time, the complaints become more severe and last longer. The duration of the complaints ranges between 2 and 4 weeks. In recurrent infection attacks, the duration is shorter and complaints are milder.
In herpes infection, blister-like (vesicular) lesions are observed on a red, hard skin in the genital area. Blister-like lesions then burst and turn into ulcers, i.e. wounds. Finally, the lesion heals by forming scabs.
Complaints of genital herpes infection include:
Frequent recurrent attacks of herpes, medications used, and abstinence from sexual intercourse can also cause some psychological problems in people.
Genital herpes infection is contagious in the period from the formation of itchy lesions on the skin to the complete healing of the ulcers. This period is 2-4 months on average. During this period, patients should abstain from sexual intercourse.
Genital herpes infection is transmitted by sexual intercourse that involves skin-to-skin contact. Since a condom does not completely cover the genital area, it can provide only partial protection; so it cannot be 100% protective. Research revealed that HSV-1 also causes infection in the genital area in consequence of oral-genital contacts.
Genital herpes is usually diagnosed by observing its characteristic lesions. Fluid-filled painful blisters on the red skin suggest the diagnosis of genital herpes. Even if it looks like other diseases, an experienced physician can diagnose these lesions by visual examination alone. In cases where the physician has difficulty making a decision or where the lesions cannot be seen with the naked eye, laboratory tests are helpful for a definitive diagnosis. These tests include;
Virological Tests: It involves the detection of the virus in the culture medium, using liquid samples taken from the lesions. It requires special transport and storage conditions. In 50% of patient groups, diagnosis can be made with this method. However, even if the test result is negative, it cannot be said that there is definitely no genital herpes infection. In detecting the virus, it is more reliable take fluid samples before the lesions dry out and form scabs. It can be easily diagnosed especially with samples taken in the first 3 days, when liquid-filled blisters occur.
PCR Test: It is the evaluation of the virus DNA with the swab taken from the lesion. Compared to virology tests, it gives faster results.
Serological Tests: It is a blood test differing from virological and PCR tests. The diagnosis is made by testing the blood to detect antibodies, which are the response of the body’s defense system against the virus. Antibodies against both types of HSV can be detected with serological tests. HSV antibodies detected in the blood indicate the existence of the virus, even if the disease is in the latent phase; and this means that the risk for infectiousness continues.
Test selection is made based on the patient’s clinical condition. In the presence of active lesions, Virological Tests and PCR are preferred. PCR is the most reliable test. However, it is not the first choice as it is an expensive technique. In recurrent infections, serological tests are performed when there are atypical lesions (in other words, if a definitive diagnosis cannot be made by eye) or when the virological test result is negative. Diagnostic serological tests are very important in cases where the patient has no obvious infection, and in determining the treatment of the sexual partner.
Especially if such lesions exist during childbirth, they can infect the baby, causing fatal diseases. Therefore, cesarean section can be preferred as the mode of childbirth delivery in pregnant women with active genital herpes. However, pregnant women who do not have an active disease at the time of childbirth can have a vaginal delivery, even if they have herpes.
It is reported that herpes infections can cause brain damage and death in newborn infants (neonatal herpes),whose immune system does not function sufficiently. Neonatal herpes has a prevalence ranging between one in 1,700 births and one in 8,200 births.
Treatment of genital herpes involves the use of antiviral drugs. These are drugs with active ingredients such as ‘Acyclovir’, ‘Famciclovir’ and ‘Valacyclovir’. Acyclovir is the oldest known antiviral drug. This treatment cannot completely eliminate HSV from the body. When started early, it can just decrease the severity and duration of the symptoms. Genital herpes treatment varies depending on whether the case involves a primary or recurrent infection.
Early detection of the symptoms is of great importance for the effectiveness of the treatment. Proliferation of the virus is prevented using antiviral drugs. In this way, complaints are reduced. However, it cannot be completely removed from the body. If the lesions keep appearing despite the initiation of treatment, the drug should be used for a period of at least 5 days. If the drug is not used uninterruptedly, it will have no effect.
Since their symptoms are not severe, they may not require antiviral treatment. Complaints can be reduced with some methods. This period can be overcome using certain methods such as applying ice to the area if the lesions are not severe, protecting the area against other infections, drinking plenty of water, and not wearing tight pants. However, if the complaints keep increasing, the patient should consult a doctor, and a treatment should be initiated.
If the number of yearly attacks is higher than 6 and if the lesions are severe, a suppressive therapy should be initiated. Treatment is long-lasting. Acyclovir treatment is administered twice a day, for a period of 6 months to 1 year. In this way, the number of attacks and the risk of infection are reduced. At the end of 1 year, the treatment is ended. When attacks repeat afterwards, 5-day short-term treatments can be administered. The frequency of attacks usually decreases after 2 years.
There is no protective vaccine for genital herpes infection and, unfortunately, it is not easy to avoid the disease. Even if there is no visible lesion, HSV can be sexually transmitted to the partner. People with active lesions or carrying the herpes virus should have awareness in this regard. Since the patient can infect her partner, she should abstain from sexual intercourse for the period that begins from the moment the lesion first appears and lasts until the wounds fully heal. It should be remembered that the disease can cause serious infections, especially in people with weak immune systems.
Although the use of condom does not provide full protection, it reduces the risk of infection to a certain extent. In addition, avoiding having multiple sex partners and making sure that the partner does not have any active lesion are some of the measures that can be taken.
Genital herpes lesions can sometimes be confused with other diseases. Genital warts, syphilis, molluscum and cancers are among them. Genital warts and syphilis lesions are usually painless. Molluscum lesions are dome-shaped small raised lumps. However, these lumps do not contain liquid. Some skin and vulva cancers may involve herpes-like lesions, as well. Therefore, when any lesion appears in the genital area, a gynecologist (for women),a urologist (for men) or a dermatologist should be consulted.
It would be appropriate for people who have had genital herpes infection to be checked for other sexually transmitted diseases.
According to a study, people with Type 2 Herpes infection are at a 3 times higher risk for HIV (AIDS) infection.
Once transmitted, HSV remains in the body for life. The treatments given cannot destroy the virus completely. In cases where the body resistance is weakened, lesions can develop repeatedly. However, development of lesions can be prevented by doing some changes in the way of life. These include;
To strengthen the immune system, it is important to sleep regularly and avoid stress. In addition, it is necessary to exercise regularly and avoid smoking. Besides these, a natural and healthy diet is a must. Ozone therapy is also among the methods used.
Some foods have been proven to strengthen the immune system. These include blueberries, bitter chocolate, turmeric, echinacea, kefir, green tea, and tea made from olive tree leaves. It would be beneficial to include these foods in the diet and to maintain weight control. Some drugs that strengthen the immune system are available on the market, as well.
In our clinic, where tests including PCR and blood tests for herpes patients are performed, all sexually transmitted diseases can be screened with a screening panel. In addition to their treatments, our patients are followed up, as well. On the other hand, we also support our patients with immune system boosting treatments such as ozone therapy.